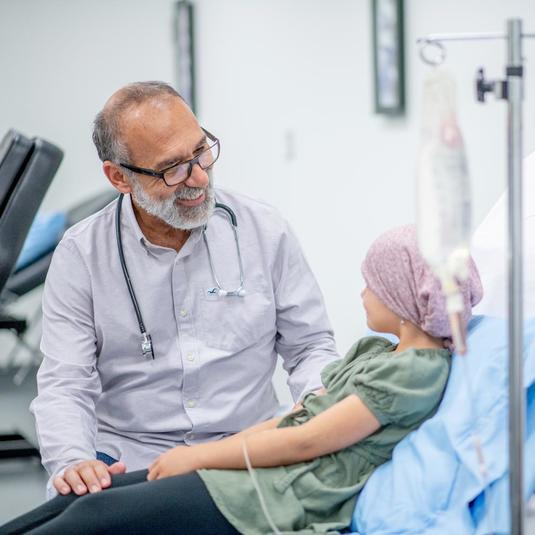
Personalized Care, Empathetic Experts
LifeBridge Health’s unique, team-based approach to cancer care prioritizes compassion in helping patients and their families navigate this life-changing diagnosis. We understand that cancer is so much more than a disease – that it presents new challenges and uncertainties which must be met with thoroughness, availability and above all, empathy.